In a recent blog we shared some highlights from our 2025 releases and now we’re celebrating over 30 years of progress with a comprehensive look back at how hundreds of families have turned to their stored cord blood as a treatment option in their healthcare journey. These releases come from the CooperSurgical owned laboratory where Cells for Life’s samples are stored (CooperSurgical is Cells for Life’s parent company).
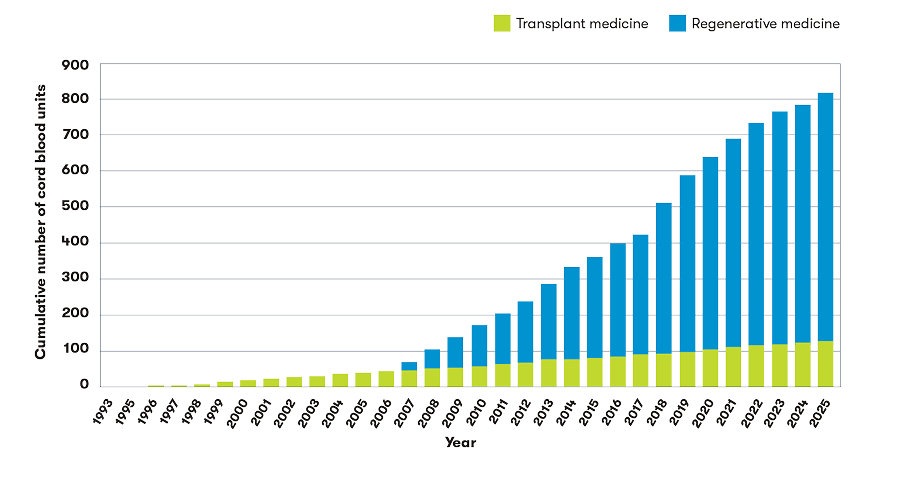
Cumulative cord blood units released
This year, we observe a significant milestone: the CooperSurgical laboratory has released more than 800 cord blood samples intended for use in transplant medicine and regulated investigational regenerative medicine uses over the last 30 years.1 The CooperSurgical laboratory has released more cord blood units than any other lab from a family bank, further solidifying its position as the world’s largest and most experienced lab in the private newborn stem cell preservation field.1
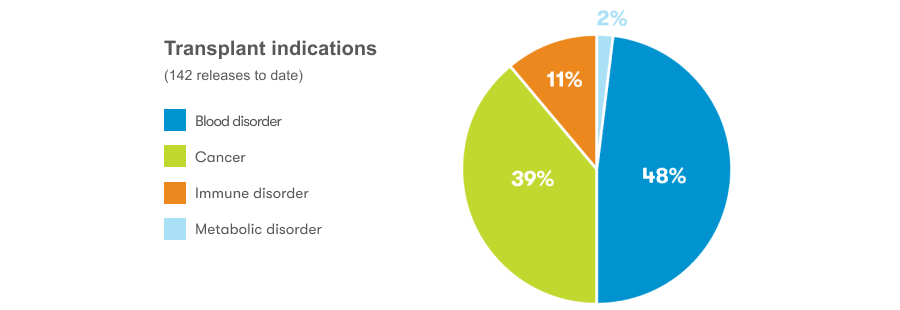
Reasons for releases
Cord blood can be used as a part of a stem cell transplant to help rebuild healthy blood and immune systems and has been used in over 50,000 transplants worldwide.2 Stem cell transplants can be used to treat more than 80 conditions,3 and CooperSurgical has released cord blood units intended to treat over 20 of these conditions.1 Some of the most common conditions that cord blood units were intended to treat include sickle cell disease, acute lymphocytic/lymphoblastic leukemia (ALL), and beta thalassemia (blood disorder).1 Blood disorders and cancers represent the largest categories of indications for transplant-related releases.
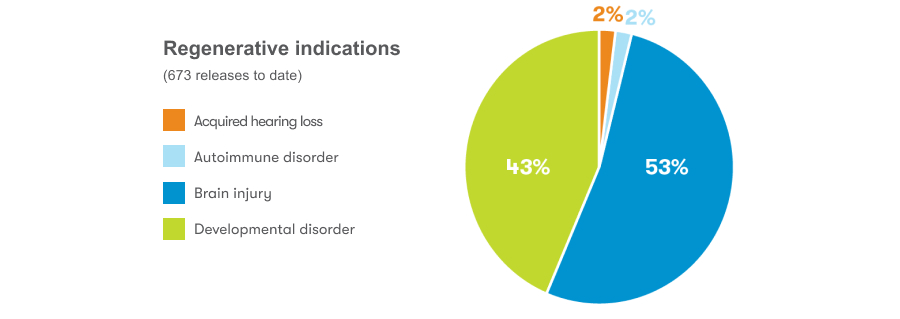
Cord blood is also being investigated in regenerative medicine for it’s potential to facilitate repair of damaged tissues and organs in the body. Approximately 83% of samples released from the CooperSurgical lab were intended for use in experimental regenerative medicine treatments. These reasons for release included approximately 30 conditions, such as cerebral palsy and hydrocephalus (excess fluid in the brain).1
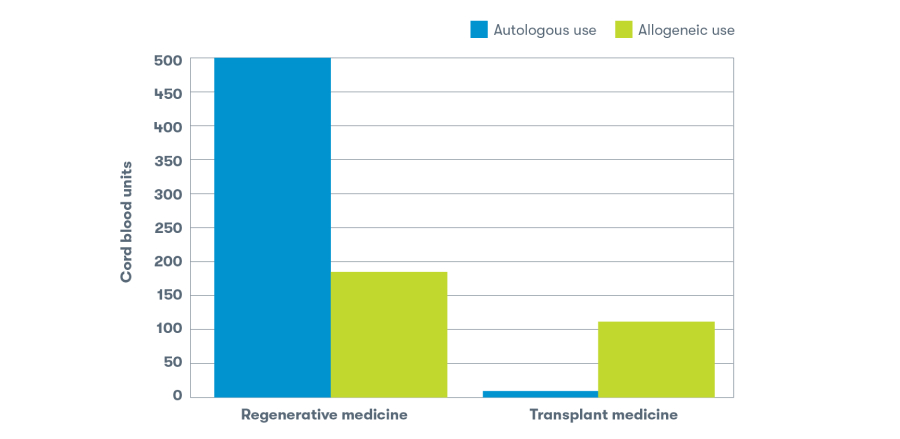
Autologous vs. allogeneic use
The decision regarding the use of autologous stem cells (patient’s own) or allogeneic stem cells (donor source) for a stem cell transplant procedure or experimental regenerative medicine treatment depends on several factors, including the specific condition being treated and the patient’s individual circumstances and medical history.4
Approximately 63% of cord blood sample releases from the CooperSurgical laboratory were intended for treatments involving the patient’s own cord blood.1 According to the release data, autologous uses are more common in experimental regenerative medicine treatments, while allogeneic uses are more commonly observed in transplant medicine. Among the allogeneic uses was one syngeneic case, a rare instance where the donor and recipient are identical twins.
Age range of samples
CooperSurgical’s specialized laboratory and storage facility has released samples ranging in storage from 11 days to 17 years, and over 200 releases have been for samples that had been in storage for 5 years or more.1 The state-of-the-art facility features 24/7 monitoring, auto-tank fill systems, regular temperature and environment checks, two 34,000-liter liquid nitrogen tanks for backup supply, and an industrial diesel emergency generator. Research has shown that proper cryostorage helps ensure that samples retain their properties for potential future use for many decades.<5
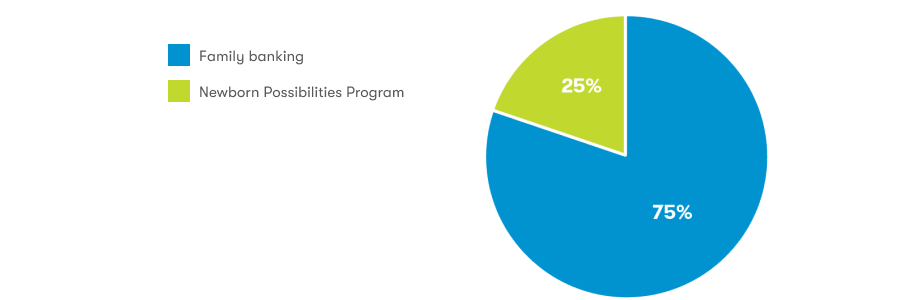
Family banking and Newborn Possibilities Program™
Newborn Possibilities Program™ – offered through Cells for Life, its parent company CooperSurgical, and other related entities – provides no-cost newborn stem cell preservation of cord blood and cord tissue, along with five years of free storage, for families with a qualifying medical need. Twenty-five percent of the samples we have released to date were for families who banked their samples under this program. With this program, Insception Lifebank is helping to expand access to potentially life-changing stem cell therapies for those who may need them the most and may otherwise not have access.
Notably, the majority of samples released were under family banking for families who did not have an identified medical need at the time of preservation. This shows that family history and diagnoses during pregnancy may not be an indicator of potential future need for newborn stem cells. This reinforces the importance for all expecting parents to be educated on their newborn stem cell preservation options.
The value of cord blood banking
For all of these families who used their cord blood sample, the value of preserving became clear when it mattered most. When their family needed cord blood for treatment, they were grateful to have this medical resource ready to support their loved one.
Expecting a child, or have friends or family who are? How about a grandchild? Enroll with Cells for Life today or refer a friend. When someone you refer preserves with Cells for Life you’ll receive a cheque or storage credit to fund your storage fees.*